J Clin Aesthet Dermatol. 2020;13(6):40–42
J Clin Aesthet Dermatol. 2020;13(6):40–42
by Christopher White, DO; Maheera Farsi, DO, FAAD; David Esguerra, DO, FAOCD; and Richard Miller, DO, FAOCD
All authors are with HCA Healthcare/University of South Florida Morsani College of Medicine at Largo Medical Center Department of Dermatology in Largo, Florida
FUNDING: No funding was provided for this study.
DISCLOSURES: The authors have no conflicts of interest relevant to the content of this article.
ABSTRACT: Pilomatrix carcinoma is a rare malignancy stemming from aberrant proliferation of matrical cells found in developing hair. This neoplasm demonstrates a bimodal age distribution and a proclivity for developing on the head or neck. Clinically, a firm, painless, violaceous nodule with overlying ulceration is commonly described. Pilomatrix carcinoma is considered a variable-grade malignancy that tends to be locally aggressive, though metastatic disease occurs in 10 to 16 percent of cases. Mortality rates range from 7 to 9 percent. Although there is no definitive treatment protocol, surgical intervention in the form of local excision or via Mohs micrographic surgery can be considered, with radiotherapy adopted as an effective alternative for nonsurgical, recurrent, or metastatic disease. Here, we describe the case of a 62-year-old man who presented for evaluation of a red, enlarging lesion on his forehead which became tender and started to bleed shortly before the patient presented to our clinic. The patient was ultimately referred to a tertiary care center for surgical excision and, at the time of this pubilcation, has been tumor-free for more than one year. This case of a rare and often unconsidered neoplasm underscores the importance of clinical suspicion and close patient follow up to prevent local recurrence, metastasis, and death.
Keywords: Pilomatrix carcinoma, malignant pilomatricoma, malignant pilomatrixoma
In the developing hair, germinative matrix cells proliferate and eventually mature and keratinize into the hair shaft and internal and external root sheaths.1 Aberrant proliferation of these matrical cells can lead to neoplasms, the most common of which is the benign pilomatrixoma. A malignant variant, termed pilomatrix carcinoma (PC) or calcified epithelial carcinoma of Malherbe, was first described by Lopansri and Mihm in 1980.2 This rare, variable-grade malignancy is locally aggressive and has a penchant for local recurrence even after securing tumor-free margins with excision.3 Though metastasis has previously been described as infrequent in the literature, emerging research suggests a more significant metastatic potential.3,4
Case Presentation
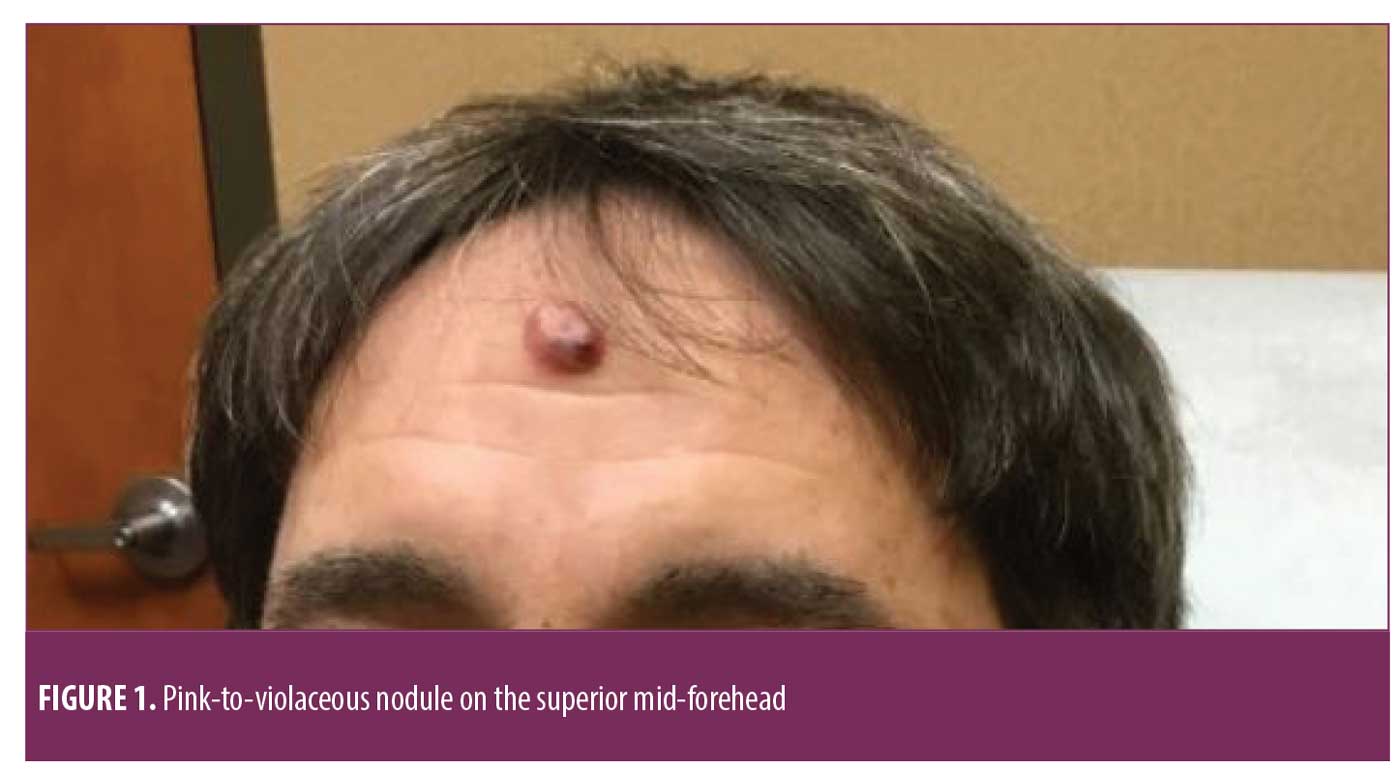
We report the case of a 62-year-old Caucasian male patient who presented to outpatient dermatology for the evaluation of an enlarging, red mass on his forehead. The lesion had erupted 8 to 10 weeks prior but had recently become tender and occasionally bled. The patient did not report any relevant medical history. Physical examination demonstrated a 3-cm smooth, pink-to-violaceous nodule in the superior mid-forehead region that was tender to palpation (Figure 1). Dermoscopy revealed focal ulceration within the nodule and frequent irregularly-shaped telangiectasias. There was no readily identified pigment network.
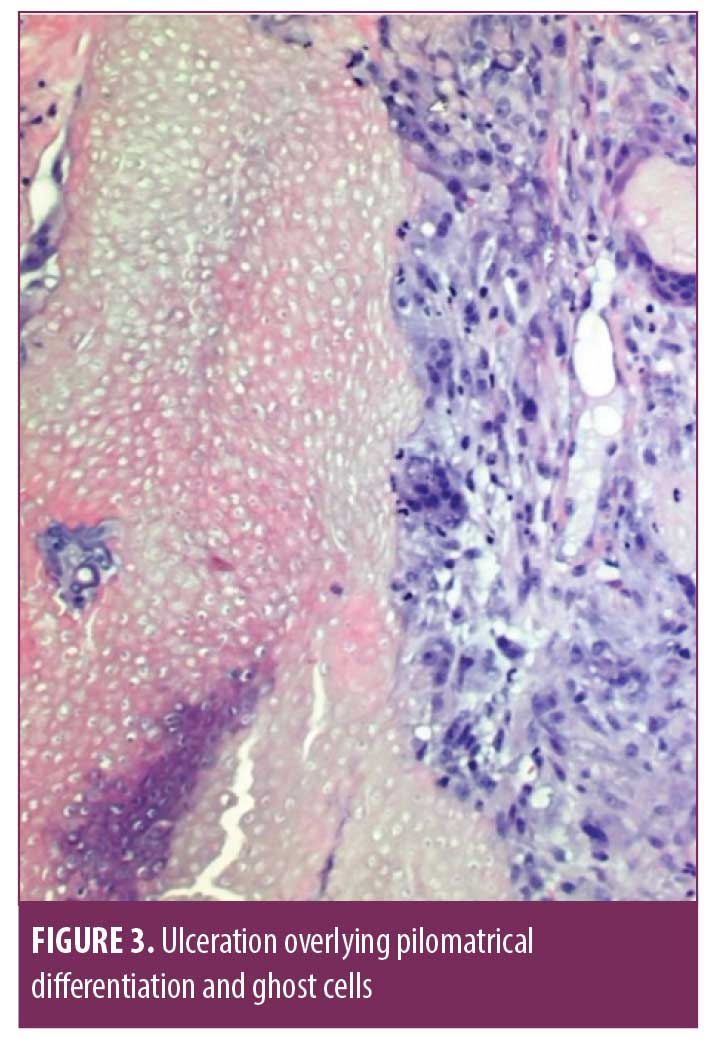
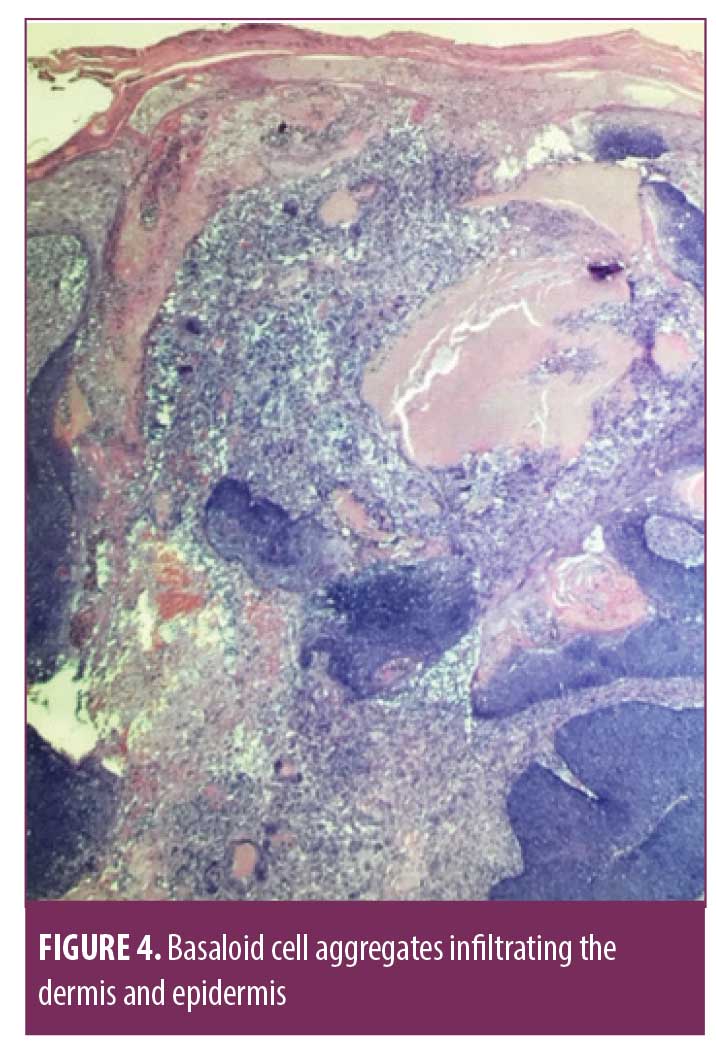
Shave biopsy was performed, with histopathology showing an asymmetrical, infiltrative epithelial proliferation within the dermis (Figure 2). Ulceration was noted with evidence of pilomatrical differentiation and ghost cells (Figure 3). Pleomorphic, basaloid cell aggregates with matrical differentiation were present, demonstrating an infiltrative growth pattern extending into the epidermis (Figure 4). These findings were consistent with pilomatrix carcinoma.

 The patient was referred to a tertiary care center and ultimately underwent Mohs micrographic surgery (MMS). Clear margins were obtained and a bilateral advancement flap was used for closure the following day. No initial or subsequent imaging was performed. The patient received biannual skin checks since undergoing MMS and remained tumor-free at the 14-month mark.
The patient was referred to a tertiary care center and ultimately underwent Mohs micrographic surgery (MMS). Clear margins were obtained and a bilateral advancement flap was used for closure the following day. No initial or subsequent imaging was performed. The patient received biannual skin checks since undergoing MMS and remained tumor-free at the 14-month mark.
Discussion
Of the 135 cases of PC that have been reported worldwide, there exists a bimodal prevalence of disease within the first three decades and the sixth to seventh decades of life.2,5 More than half of these malignancies occur on the head and neck, with a male-to-female disease ratio of 3:1.5,6 While most tumors will remain localized, in the 10 to 16 percent of cases where metastasis occurs, at least 60 percent of these arise in men; the most frequently affected organs are regional lymphatics, the lungs, or bone.5,7
While both de novo PC formation and malignant transformation of pre-existing pilomatrixomas have been described, the presence of a common CTNNB1 gene mutation in both neoplasms suggests a shared pathogenesis.2,8,9 Functionally, this gene codes for beta-catenin, a cytoskeletal and cell-signaling protein that serves a role in the downstream WNT signaling pathway.1,6,10 Exon 3 of CTNNB1 encodes the phosphorylation site of beta-catenin, which normally marks the structure for degradation, providing that the WNT ligand is absent.4,10 This checkpoint is averted through mutation, precluding the WNT gatekeeping function.11–13 Cytoplasmic beta-catenin freely translocates to the nucleus, where it serves as a cofactor for the T-cell factor/lymphoid-enhancing factor (LEF) transcription factors, upregulating transcription factors, such as LEF1, which has roles in both hair cell differentiation and follicular morphogenesis.1,4,12 The nuclear accumulation of beta-catenin can be used as a surrogate marker of CTNNB1 mutation, which is found in both pilomatrixomas and pilomatrix carcinomas.13 Comparatively, other adnexal structures accumulate beta-catenin, appropriately, within the cytoplasm alone.
As similar mutations are present in pilomatrixomas and PC, the two-hit hypothesis is suspected, with the first mutation responsible for initial nuclear beta-catenin accumulation and the second mutation conveying malignant potential.4,9,10 Considering the propensity for these tumors to present on the neck and head, photodamage via ultraviolet light might supply the requisite second mutation.5,14 Interestingly, a specific genetic defect has not been identified in the development of pilomatrixomas, though multiple disease processes display a predisposition for developing this rare neoplasm (e.g., xeroderma pigmentosum; Turner, Gardner and Rubinstein-Taybi syndromes).2,10
Clinical characteristics. Pilomatrix carcinoma frequently presents as a single asymptomatic dermal or subcutaneous mass that is firm, painless, and mobile.2,5,14 Violaceous discoloration and ulceration of the overlying skin has been reported, the latter of which is considered one of the only notable signs of malignancy.1,3,15 This nonspecific description potentially explains the infrequent clinical diagnosis of PC, with one review stating that, of 20 reported cases, none were initially diagnosed as PC.2,7 The most frequently implicated differential diagnoses include basal cell carcinoma, epidermal cyst, amelanotic melanoma and pilomatrixoma.4,13,15 Though PC is rarely suspected clinically, biopsy is often performed due to rapid tumor growth either de novo or as an evolution of a previously stable lesion.6 The speed of growth is more predictive of malignancy than overall size, with the literature reporting malignant tumors ranging from 0.5 to 4cm in size.3,5,10
Histopathology. Grossly, excised tumors are often asymmetric, encapsulated, and cystoid, with a grayish surface and viscous contents.16,17 Histologically, there exists a predominant dermal proliferation of basaloid cells with abundant clear cytoplasm and an abrupt transition to eosinophilic ghost or shadow cells (anucleate matrical corneocytes).6,14,17 Basaloid cells aggregate in nests, bands, and irregular sheets that rarely palisade or contain melanin.7,17 Ulceration and calcification are interspersed between cell types.5,10,16 Nuclei of the basaloid cells are pleomorphic, with frequent, atypical mitoses and a high apoptotic index.4,6,16 Ulceration and infiltration into adnexal structures strongly support diagnosis, with some reports even correlating these findings with the degree of malignancy.8,17 Dense desmoplastic stroma with a lymphohistiocytic infiltrate is typically located adjacent to the tumor capsule.6,17
Immunohistochemistry. While not required, a variety of immunohistochemical analyses can be used to support the diagnosis of PC. The most frequently utilized profiles target beta-catenin, LEF1, B-cell lymphoma 2 (Bcl-2), Bcl-2–associated X protein (BAX), and cluster of differentiation (CD)44.16 Pan-cellular staining for LEF1 and beta-catenin is strictly observed in the pilomatrixoma and PC in contrast with in tumors with focal germinative matrix cell nests, such as basal cell carcinoma and trichoblastoma, which show staining confined to these areas.1,10 The CD44 isoforms have been found by some researchers to directly relate to metastatic potential, whereas a high ratio of BAX to Bcl-2 correlated with a good prognosis and even predicted a high sensitivity to radiation.16 While diffuse beta-catenin and LEF1 staining narrows the differential diagnosis to tumors of pilomatrix origin, they make no distinction between benign and malignant variants. Thus, PC remains a histologic diagnosis aided, but not confirmed, by immunohistochemistry.3,5,10 Though, since beta-catenin indicates cellular maturation, it is speculated that lower levels of this marker more likely signal metastases.16
Treatment and prognosis. Due to the infrequency with which PC occurs, there exist no concrete guidelines concerning treatment protocol. Most authors agree on performing local excision with margins ranging from 5 to 30mm, as this approach poses the lowest risk of recurrence.2,8 Interestingly, reported metastases occurred equivalently in tumors excised using both simple and wide approaches.5,10 Newer literature suggests that MMS might offer the highest cure rate, with superior margin control and improved cosmetic outcomes.2,4–6,8 In cases where surgery is either impossible or does not afford adequate margins, radiotherapy is extremely effective, with no progression of disease following its use; adjuvant radiation is appropriate in cases of recurrent or metastatic disease.2,3,6,8 Chemotherapy has been reported to be generally ineffective.2,3,5,6
The overall prognosis in PC is primarily dependent on identification of the suspicious lesion along with the initial treatment approach. In cases treated with simple excision, 50 to 83 percent of lesions locally recurred, while widely excised lesions returned in 18 to 23 percent of patients.5,6,10,17 Metastases occurred in 10 to 16 percent of cases and most frequently affected lymphatic or pulmonary structures.2,4,6 Death was reported as a direct or indirect result of PC in 7 to 9 percent of patients.5,6 Due to the high frequency of local recurrence and the risk of metastasis, it is recommended that patients with confirmed cases of PC be scheduled for total-body skin examination 2 to 3 times annually.2,5
References
- Battistella M, Carlson J, Osio A, et al. Skin tumors with matrical differentiation: lessons from hair keratins, beta-catenin and PHLDA-1 expression. J Cutan Pathol. 2014;41(5):427–436.
- Jones C, Twoon M, Ho W, et al. Pilomatrix carcinoma: 12-year experience and review of the literature. J Cutan Pathol. 2018;45(1):33–38.
- Papadakis M, Bree E, Floros N, et al. Pilomatrix carcinoma: more malignant biological behavior than was considered in the past. Mol Clin Oncol. 2016;6(3):415–418.
- Cornejo K, Deng A. Pilomatrix carcinoma: a case report and review of the literature. Am J Dermatopath. 2013;35(3):389–394.
- Melancon J, Tom W, Lee R, et al. Management of pilomatrix carcinoma: a case report of successful treatment with Mohs micrographic surgery and review of the literature. Dermatol Surg. 2011;37(12):1798–1805.
- Herrmann J, Allan A, Trapp K, et al. Pilomatrix carcinoma: 13 new cases and review of the literature with emphasis on predictors of metastasis. J Am Acad Dermatol. 2014;71(1):38–43.
- Otero M, Trujillo C, Parra-Medina R, et al. Metastatic malignant pilomatrixoma in an 8-year-old girl misdiagnosed as a recurrent pilomatrixoma. Am J Dermatopathol. 2017;39(3):e41–e43.
- Karaaslan O, Can M, Silistreli A, et al. Malignant pilomatrixoma arising on the previously irradiated face: case report and literature review. J Cutan Surg. 2012;16(5):341–343.
- Hassanein A, Glanz S. Beta-catenin expression in benign and malignant pilomatrix neoplasm. Br J Dermatol. 2004;150(3):511–516.
- Lazar A, Calonje E, Grayson W, et al. Pilomatrix carcinomas contain mutation in CTNNB1, the gene encoding beta-catenin. J Cutan Pathol. 2005;32(2):148–157.
- Nishioka M, Tanemura A, Yamanaka T, et al. Pilomatrix carcinoma arising from pilomatricoma after 10-year senescent period: immunohistochemical analysis. J Dermatol. 2010;37(8):735–739.
- Soler A, Kindel S, McCloskey G, et al. Cell–cell adhesion proteins in melanocytic pilomatrix carcinoma. Rare Tumors. 2010;2(3):e43.
- Bailey E, Rushovich A, Kim J. A growing nodule on the forearm of an 84-year-old man. J Cutan Pathol. 2017;44(1):1–4.
- Bolognia J, Schaffer J, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier, 2018.
- Walker D, Dowthwaite S, Cronin D, et al. Metastatic pilomatrix carcinoma: not so rare after all? A case report and review of the literature. Ear Nose Throat J. 2016;95(3):117–120.
- Bassarova A, Nesland J, Sedloev T, et al. Pilomatrix carcinoma with lymph node metastases. J Cutan Pathol. 2004;31(4):330–335.
- Hardisson D, Linares M, Cuevas-Santos J, et al. Pilomatrix carcinoma: a clinicopathologic study of six cases and review of the literature. Am J Dermatopath. 2001;23(5):394–401.
- Thomas C, Wood G, Marks V. Mohs micrographic surgery in the treatment of rare aggressive cutaneous tumors: the Geisinger experience. Dermatol Surg. 2007;33(3):333–339.