J Clin Aesthet Dermatol. 2020;13(5):48–53
J Clin Aesthet Dermatol. 2020;13(5):48–53
by Paul Macklis, MS; Kevin Adams, BA; Jessica Kaffenberger, MD; Purnima Kumar, BDS MS PhD; Andrew Krispinsky, MD; and Benjamin Kaffenberger, MD
Mr. Macklis is with the Ohio State University College of Medicine in Columbus, Ohio. Mr. Adams with with the University of Toledo College of Medicine in Toledo, Ohio. Dr. Kumar is with the Division of Periodontology at the Ohio State University College of Dentistry in Columbus, Ohio. Drs. J. Kaffenberger, Krispinsky, and B. Kaffenberger are with Ohio State University Wexner Medical Center in Columbus, Ohio.
FUNDING: This work was supported in part by the OSU College of Medicine Bennett research scholarship
DISCLOSURES: The authors have no conlflicts of interest relevant to the content of this article.
ABSTRACT: Objective. Oral health and mucocutaneous inflammation might play an important role in the etiopathogenesis of many skin diseases, especially those that also involve the oral mucosa. This review examines the relationship between skin conditions and various oral health metrics to better understand how oral diseases, especially periodontitis, might influence the development or prognosis of several conditions, including aphthous stomatitis, atopic dermatitis, lichen planus, pemphigus, pemphigoid, and psoriasis.
Methods. Using the PubMed search engine between Summer 2017 and Summer 2018, searches were performed for: oral health OR oral hygiene AND psoriasis, eczema, dermatitis, hidradenitis suppurativa, acne inversa, pyoderma gangrenosum, Sweet’s syndrome, neutrophilic dermatosis, subcorneal pustular dermatosis, hives, urticaria, cutaneous lupus, pemphigoid, pemphigus, or lichen planus OR aphthous stomatitis. The abstract of articles written in English were reviewed by the investigators and selected for inclusion if the study involved a correlation between oral health/hygiene and skin disease. After studies were included, the references were reviewed for additional relevant studies. Diseases listed in the search terms that were not ultimately discussed in this review did not produce any articles of relevance.
Results. Aphthous stomatitis is correlated with poor periodontal health and greater plaque accumulation. Atopic dermatitis shows an association with gingivitis, toothaches, and oral infections. Heavier enamel plaque burden and reduced oral care are implicated in the exacerbation of lichen planus. Mucous membrane pemphigoid and pemphigus are intimately influenced by oral health, underscoring the important role of good oral health and hygiene. Psoriasis presents a strong connection with oral streptococcal bacterial burden, has been shown to be improved or even cured with tonsillectomy, and has treatment outcomes that are generally associated with periodontal disease.
Conclusion. Comorbid disease associations are frequently being reported in dermatology, spurring collaboration between multiple specialists and dermatologists. This review emphasizes a need for closer collaboration between dermatologists and dentists to treat several common skin diseases.
Keywords: Oral hygiene, oral health, aphthous stomatitis, dermatitis, eczema, lichen planus, pemphigoid, pemphigus, psoriasis
Periodontitis is an infectious disease caused by dysbiotic microbial communities in the subgingival sulcus, leading to the destruction of structures that anchor the tooth to the jawbone and subsequent loss of the tooth or teeth. The subgingival sulcus is a physiological space between the tooth and the surrounding gingiva containing nearly 10 million organisms, representing 70 to 150 different species in each individual.2 Changes in this environment can lead to dysbiosis in the indigenous microbiome, reducing the abundance of the commensal population and creating a pathogen-rich ecosystem.3 The florid immune-inflammatory response to this pathogenic colonization leads to the destruction of the attachment between the tooth and the gingiva, along with the loss of structures that support and sustain the tooth. Together, these two events result in a deepening of the gingival sulcus, which provides an ideal environment for anaerobe colonization, including many organisms that are pathogenic.4 The diseased periodontal pocket also contains significant levels of inflammatory mediators, including tumor necrosis factor alpha (TNF-?), interleukin (IL)-1, IL-2, and IL-8, and prostaglandins (PGEs), which can be released into the circulation from the diseased periodontium and can contribute to systemic inflammation.5
Periodontitis shows evidence of systemic inflammation with elevated C-reactive protein levels in both acute and chronic cases.6 One of the most substantial contributing factors is the presence of dental plaque, which is most commonly removed via brushing and flossing.7 Oral health can be heavily influenced by behavior, and poor oral hygiene can produce dramatic changes in the oral microbiome.8
While the oral microbiome is diverse and robust, a number of bacterial species have been associated with health, including several species of Streptococci (notably Streptococcus salivarius [S. salivarius], S. mitis, S. oralis, and S. sanguinis) as well as bacteria from the Veillonella and Actinomyces genuses.2 Conversely, the presence of Acholeplasma, Fretibacterium, Porphyromonas gingivalis, Peptococcus, Treponema denticola, Defluviitaleaceae_UCG_011, Filifactor, and Mycoplasma were associated with periodontal disease.9 Though these species were also present in the oral cavities of healthy patients, they were enriched in regions of periodontal disease and increased in accordance with periodontal pocket depth, a measurement of periodontal disease severity. Numerous studies have identified connections between oral hygiene, the presence of specific bacterial species, and a variety of autoimmune skin conditions suggesting that oral care and its subsequent effect on the oral microbiome could be a modifiable risk factor for these conditions. This article provides a summary of the findings regarding the correlation between oral health, oral care practices, and skin disease.
Methodology
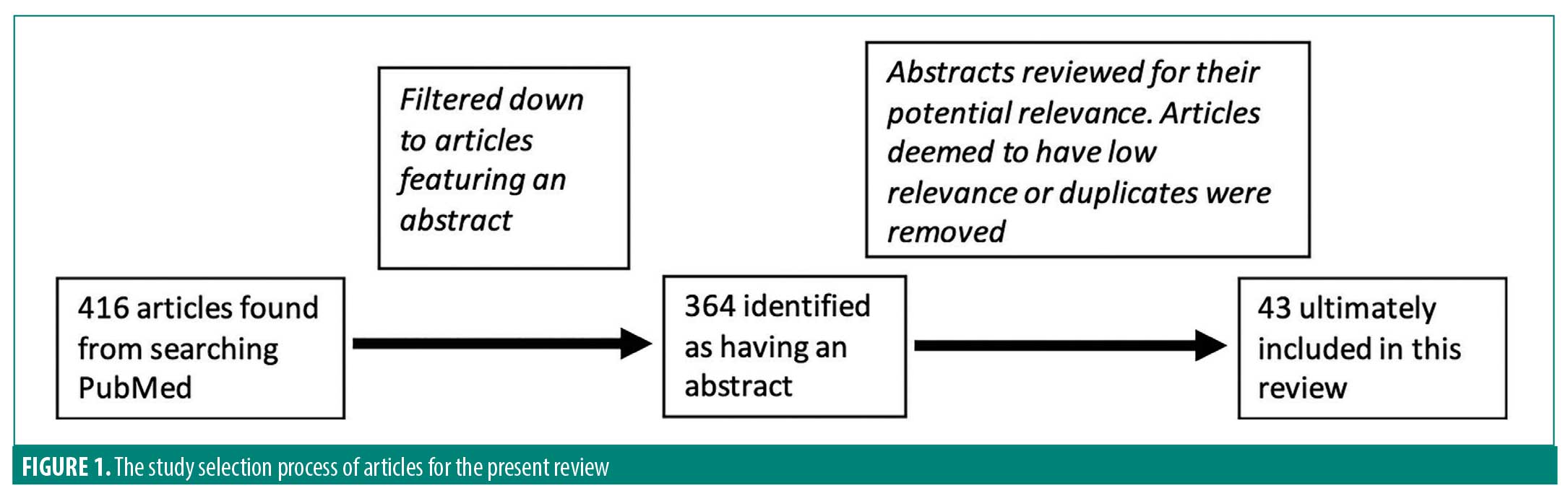
Journal articles were searched and selected to create an overview of the correlation between oral health and skin disease. Using the PubMed search engine between Summer 2017 and Summer 2018, searches were performed for: oral health OR oral hygiene AND psoriasis, eczema, dermatitis, hidradenitis suppurativa, acne inversa, pyoderma gangrenosum, Sweet’s syndrome, neutrophilic dermatosis, subcorneal pustular dermatosis, hives, urticaria, cutaneous lupus, pemphigoid, pemphigus, or lichen planus OR aphthous stomatitis. The abstract of articles written in English were reviewed by the investigators and selected for inclusion if the study involved a correlation between oral health/hygiene and skin disease (Figure 1). After studies were included, the references were reviewed for additional relevant studies. Diseases listed in the search terms that were not ultimately discussed in this review did not produce any articles of relevance. Forty-three articles were ultimately included in this review.
Results and Discussion
Aphthous stomatitis. Compared to healthy controls, patients with aphthous stomatitis had inferior oral health, with improvements in their oral health correlated with disease improvement. Larger plaque index scores, reduced tooth brushing, and oral infections showed a significant correlation with recurrent aphthous stomatitis.10 In a study that rated oral health based on metrics such as plaque, bleeding, gingival indices, probing depth, and hygienic indices, scores were significantly higher in patients with aphthous stomatitis, indicating poorer oral health.11 Self-reported poor oral health has also been associated with more severe symptoms.12
While oral health might contribute to aphthous stomatitis etiology in numerous ways, one study of 35 patients suggested that an increase in Bacteroidales within the oral mucosa might stimulate the development of aphthous stomatitis, while Porphyromonadaceae and Veillonellaceae bacteria were enriched at active lesion sites.13 These microbes were also seen in healthy mouths, but were substantially more common in the mouths of patients with aphthous stomatitis. To verify that these microbial imbalances are attributable to legitimate microbiome differences rather than pain-associated changes in brushing habits, participants adhered to a strict dietary and oral hygiene regimen for 72 hours prior to the sampling. Based on these studies, a combination of plaque accumulation, oral infections, and general poor periodontal status were all associated with aphthous stomatitis.
Dermatitis/eczema. The evidence relating oral diseases to dermatitis or eczema is equivocal. Several studies have strongly suggested a correlation between dermatitis and odontogenic infections or gingival bleeding. In one study, 30 percent of individuals with atopic dermatitis resistant to conventional treatment demonstrated periapical root infections.14 The dermatitis resolved following treatment of this odontogenic infection. In another study of 91,642 children aged 0 to 17 years, a strong correlation was found between self-reported bleeding gums in the previous six months and eczema. Moreover, severe eczema was associated with a higher prevalence of bleeding gums in univariate (12.6% vs. 4.3%; p=0.0007) and multivariate models.15 This study controlled for age, sex, race, ethnicity, household size, and educational attainment of the most educated household member. Additionally, there are several case reports available of corticosteroid-resistant chronic pigmented purpura that resolved following treatment of periodontitis, pulpitis, or both.16–18
Dermatitis has sometimes been attributed to an allergic reaction to dental amalgam, a mixture of metal alloys used in dental fillings often blamed as a potential initiating factor of allergic disease due to its mercury content.19 However, a study involving 137 Swedish teenagers found no correlation between the number of filled dental caries and allergic disease, including dermatitis.20 Additionally, this study did not report any detrimental effects of dental amalgam on the prevalence or severity of eczema.
The hygiene hypothesis, which postulates that early exposure to a suite of friendly microbes or commensals is important to train the immune system, has been proposed to explain the connection between periodontal disease and dermatological diseases. There is evidence to suggest that this exposure might occur both perinatally as well as prenatally. Indeed, some evidence has linked maternal periodontal disease to childhood impairment of the innate immune system.21 Inadequate microbial exposure prevents a shift from a Th-2–mediated cytokine-dominated response to a Th-1–mediated cellular response. Another paradigm suggests that early exposure to bacteria enables efficient training of T-regulatory (Treg) cells, which control Th cells, thereby mitigating the innate immune system. The early training of the innate immune system by oral bacteria can therefore influence the adaptive immune response to pathogens, both oral and nonoral, and thereby the phenotype of the inflammatory response. Another hypothesis is that of cross-reactivity. It has been hypothesized that focal oral infections might contribute to dermatitis through the generation of heat-shock proteins and that cross-reactivity between bacterial heat-shock proteins and human Hsp60 can produce immunogenic effects systemically.22
Lichen planus. A strong correlation between the prevalence of periodontitis and lichen planus has been demonstrated.23 The connection between poor oral health and lichen planus was also evident in a study of 30 patients with oral lichen planus that had poorer periodontal health than 30 controls across several key metrics—specifically, the gingival index, periodontal index, and bleeding on probing.24 Moreover, several periodontal pathogens, notably, Aggregatibacter actinomycetemcomitans, Porphyromonas gingivalis, Prevotella intermedia, Tannerella forsythia, and Treponema denticola have been identified at higher frequencies in subjects with oral lichen planus.25
However, a study of 90 oral lichen planus patients and 52 control patients found that periodontal status is not worse in patients with oral lichen planus, although lichen planus patients exhibited greater plaque and calculus deposits than healthy controls.26 Multiple studies suggest that poor oral hygiene, including increased plaque burden, can exacerbate lichen planus. In a Chinese study of 674 patients, it was found that oral lichen planus was exacerbated by a host of factors, including stress, foods, systemic illness, and poor oral hygiene.27 Another study of 95 patients with oral lichen planus found that 77 patients experienced exacerbations in response to stress, spicy foods, and poor oral hygiene.28
Improvements in oral hygiene dramatically improved oral lichen planus. Patients followed an intensive program that emphasized the frequency and technique of brushing; the use of interdental brushes, toothpicks, dental floss, mouth-rinsing; and the pursuit of dental cleanings for one year.29 While the majority of patients initially reported pain during tooth-brushing or eating, these symptoms dissipated in nine of the 11 patients by the end of the study in addition to observing improvements in lichen planus in the majority of patients. However, lichen planus is a mucocutaneous disease with oral manifestations. Therefore, it is difficult to determine if poor oral hygiene is secondary to the pain and discomfort experienced by the patients or if it contributed to the etiopathogenesis of the disease. Prospective longitudinal studies are required to elucidate the contributions of poor oral hygiene to the etiology of lichen planus.
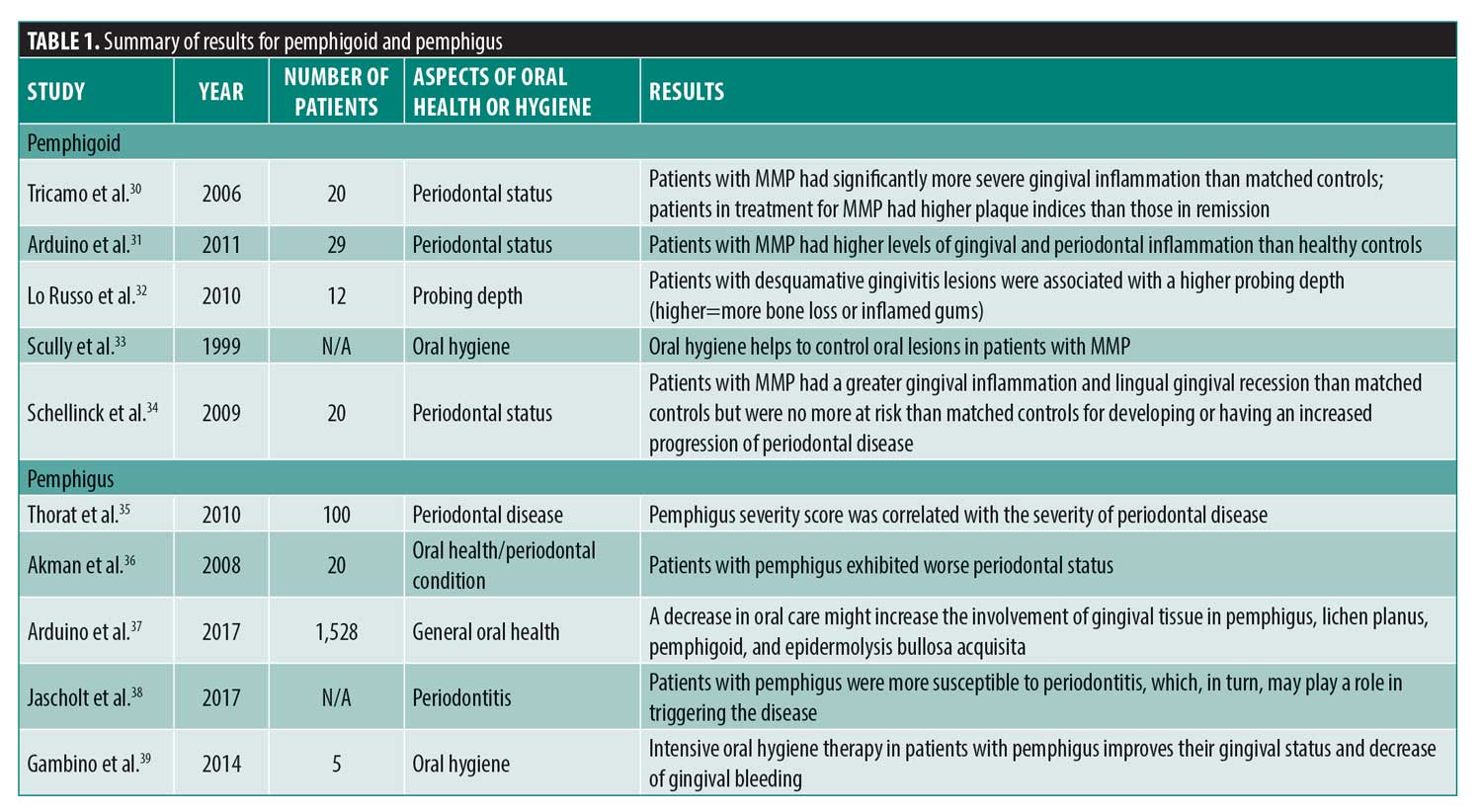
Pemphigoid. Like lichen planus, mucous membrane pemphigoid (MMP) also shows oral lesions as part of the disease complex. Patients with pemphigoid were found to have more severe gingival index scores than healthy patients, indicating more gingival inflammation.30 Although the higher gingival index could be at least partially attributed to MMP lesions, a number of linear lesions were also observed at the gingival margin, indicating that they are derived from plaque-associated gingivitis rather than MMP. Patients affected by MMP have also been found to have higher levels of both gingival and periodontal inflammation.31 Patients with MMP undergoing therapy because of active disease were also found to have more plaque than those in remission.30 MMP can often lead to desquamative gingivitis, the lesions of which have been implicated as a possible risk factor for periodontitis as well as the primary oral feature of MMP.24 Additionally, it was found that conditions similar to MMP, such as lichen planus, also saw an improvement in desquamative gingivitis following an improvement in oral hygiene.33 Another study showed that patients with MMP had a higher gingival index as well as lingual gingival recession, a common feature of periodontal disease, compared to healthy controls.34 However, patients with MMP and controls matched for age, sex, and smoking history demonstrated significant periodontal disease progression over the five-year course of the study, suggesting that patients with MMP are not at an increased risk for periodontal disease development or progression.34 Four of the 10 patients with MMP included in this study were in remission and it was noted that the erythematous nature of MMP could be responsible for the significant increase in the gingival index, especially since scores on other periodontal health measures, such as the bleeding index, were not elevated among patients with MMP.
While this study seems to contradict the numerous others that have demonstrated a connection between MMP and periodontal health, it should be noted that these findings stem from a small study of only 20 patients and did not control for the oral maintenance practices of the patients. Thus, numerous studies support the conclusion that MMP is intimately influenced by periodontal disease, underscoring the important role of good oral health and hygiene in the prevention of MMP. While patients and dentists often request clearance to perform routine dental cleanings on patients with pemphigoid, the little evidence available suggests that patients with pemphigoid should be encouraged to continue routine dental evaluations and cleanings.
Pemphigus. Pemphigus was found to be associated with several indicators of poor periodontal health, including validated indices such as the Community Periodontal Index of Treatment Needs (CPITN). Moreover, the Clinical Severity Score (CSS) of pemphigus correlated well with periodontal pocket depths and attachment loss.35 Having a diagnosis of pemphigus for longer than five years was also correlated with more severe periodontal disease.36 It has been suggested that a decrease in periodontal care might increase the involvement of gingival tissue in pemphigus, lichen planus, pemphigoid, and epidermolysis bullosa acquisita.37 These findings might be confounded by oral lesions possibly limiting an individual’s ability to perform efficient plaque control. However, several measures of periodontal disease severity, including CPITN score, probe depth, and attachment loss, were correlated with the prevalence of pemphigus, indicating that this association extends beyond poor oral hygiene.
A systematic review of 10 studies reported that the relationship between periodontitis and pemphigus/pemphigoid appears to be bidirectional, with periodontitis increasing the severity of pemphigus and patients with pemphigus being more susceptible to periodontitis.38 One week of professional oral hygiene therapy, including supragingival scaling, polishing, chlorhexidine mouth rinses, and toothbrushing, has been shown to improve the gingival status in a small sample of patients with pemphigus. Specifically, it resulted in a reduction of the full-mouth bleeding score, demonstrating a significant correlation with a reduced Oral Pemphigus Clinical Score.39 Similar to oral lichen planus, available evidence suggests patients with pemphigus should be encouraged to seek professional periodontal care and instructed in methods to maintain meticulous oral hygiene.
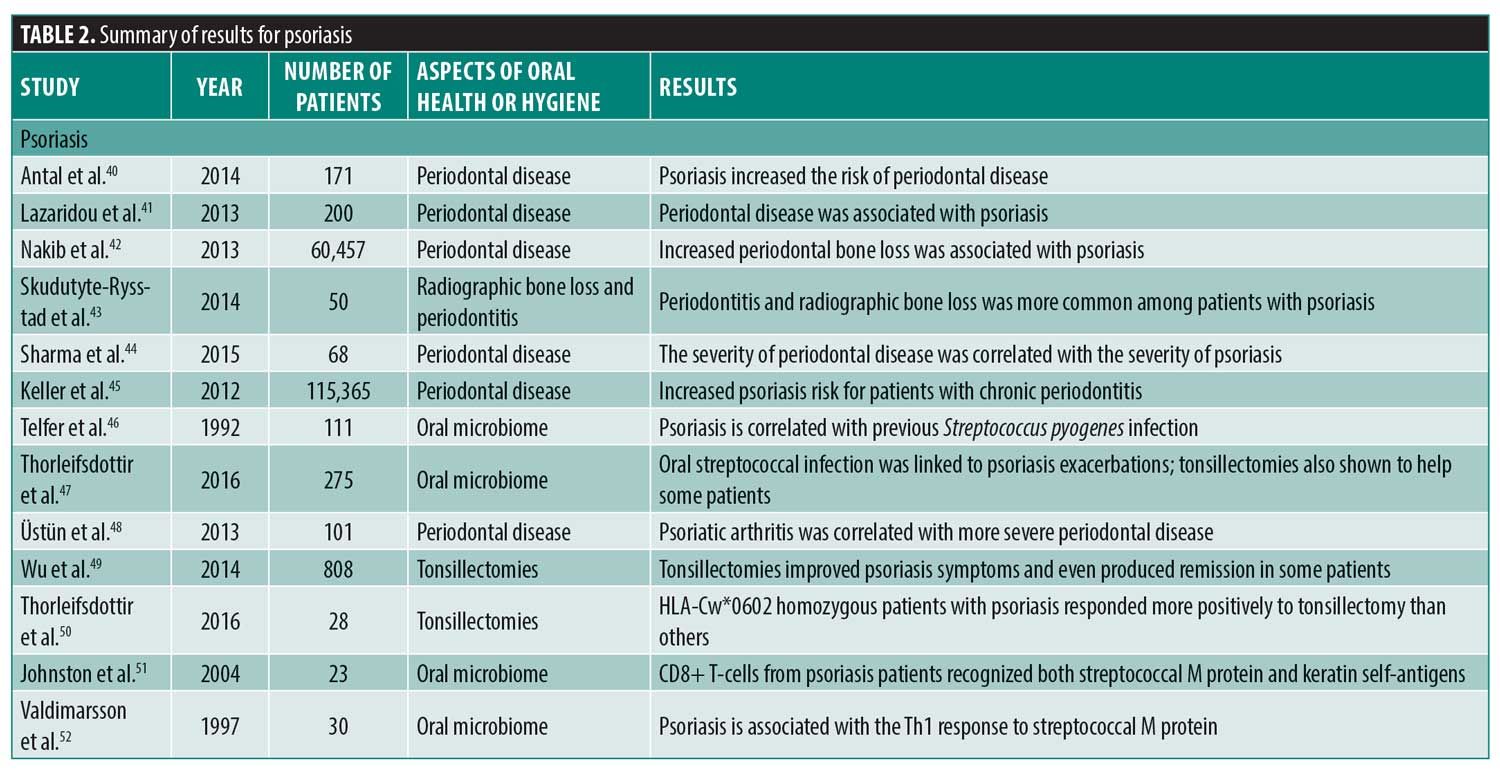
Psoriasis. Among the chronic cutaneous diseases, the strongest correlations have been observed between periodontitis and psoriasis. Patients with psoriasis demonstrate significantly greater odds of periodontitis (odds ratio: 3.329-4.373),40–44 while concomitant smoking increased the odds ratio to 24.278.40 A large study of 60,457 women revealed that the risk for psoriasis was greater in patients with mild (relative risk: 1.35, 95% confidence interval: 1.03-1.75) and moderate-to-severe periodontal bone loss (relative risk: 1.49, 95% confidence interval: 1.08-2.05) when compared to those without periodontal bone loss, after adjusting for age, cigarette smoking, body mass index, alcohol intake, physical activity, and tooth loss.42 Moreover, the surgical treatment of periodontitis served to attenuate the clinical manifestations of psoriasis.45
The oral microbiome has been implicated in the causal pathway of psoriasis. Psoriasis patients often suffer frequent streptococcal infections and 58 percent of patients affected by guttate psoriasis also had concomitant Streptococcus pyogenes infection.46 Exacerbations in psoriatic lesions have been correlated with streptococcal tonsillitis47 and periodontitis,48 indicating a potential contribution of the oral microbiome to the disease etiology. A review of 13 studies, including a total of 808 patients with psoriasis who had undergone tonsillectomies, found the majority of patients in the study experienced improvement, with some patients demonstrating complete remission.49 This was further confirmed by a recent study in which the benefit of tonsillectomy was demonstrated in patients with homozygous HLA-Cw*0602 psoriasis, a genotype that was also correlated with frequent streptococcal infections.50 Certain Streptococci produce streptococcal M protein, which shares many structural similarities with human epidermal keratins. It is believed that this cross-reactivity might play a role in the pathogenesis of psoriasis.51,52
Conclusion
Periodontal disease, especially chronic periodontitis, appears to play a role in many dermatologic diseases, although the mechanism is currently unclear. While the results have not been completely consistent, the majority of evidence supports the idea that improvements in periodontal health positively influence the diseases discussed. Overall, these findings suggest that commensal bacteria associated with periodontal health might act as a protective measure and that dysbiotic biofilms associated with periodontitis might contribute to dermatological diseases either directly or by stimulating immunoinflammatory pathways.
References
- Loesche WJ. Dental Caries: A Treatable Infection. Grand Haven, MI: ADQ Publications; 1993.
- Aas JA, Paster BJ, Stokes LN, et al. Defining the normal bacterial flora of the oral cavity. J Clin Microbiol. 2005;43(11):5721–5732.
- Socransky SS, Haffajee AD. Periodontal microbial ecology. Periodontol 2000. 2005;38:135–187.
- Listgarten MA. Pathogenesis of periodontitis. J Clin Periodontol. 1986;13(5):418–430.
- Offenbacher S, Heasman PA, Collins JG. Modulation of host PGE2 secretion as a determinant of periodontal disease expression. J Periodontol. 1993;64(5 Suppl):432–444.
- Bansal T, Pandey A, D D, Asthana AK. C-reactive protein (CRP) and its association with periodontal disease: a brief review. J Clin Diagn Res. 2014;8(7):ZE21–ZE24.
- Fleming EB, Nguyen D, Afful J, et al. Prevalence of daily flossing among adults by selected risk factors for periodontal disease—United States, 2011–2014. J Periodontol. 2018;89(8):933–939.
- Okuda K, Ebihara Y. Relationships between chronic oral infectious diseases and systemic diseases. Bull Tokyo Dent Coll. 1998;39(3):165–174.
- Shi M, Wei Y, Hu W, et al. The subgingival microbiome of periodontal pockets with different probing depths in chronic and aggressive periodontitis: a pilot study. Front Cell Infect Microbiol. 2018;8.
- Mumcu G, Ergun T, Inanc N, et al. Oral health is impaired in Behçet’s disease and is associated with disease severity. Rheumatology (Oxford). 2004;43(8):1028–1033.
- Koridze K. [Definition of risk of the aphthous stomatitis by hygienic indices]. Georgian Med News. 2005;(121):25–28. Article in Russian.
- Kojima A, Ekuni D, Mizutani S, et al. Relationships between self-rated oral health, subjective symptoms, oral health behavior and clinical conditions in Japanese university students: a cross-sectional survey at Okayama University. BMC Oral Health. 2013;13(1):62.
- Hijazi K, Lowe T, Meharg C, et al. Mucosal microbiome in patients with recurrent aphthous stomatitis. J Dent Res. 2015;94(3 Suppl):87S–94S.
- Igawa K, Nishioka K, Yokozeki H. Odontogenic focal infection could be partly involved in the pathogenesis of atopic dermatitis as exacerbating factor. Int J Dermatol. 2007;46(4):376–379.
- Silverberg JI, Simpson EL. Association between severe eczema in children and multiple comorbid conditions and increased healthcare utilization. Pediatr Allergy Immunol. 2013;24(5):476–486.
- Ceki? Arambašin A, Sistig S, Vu?i?evi? Boras V. Connection between the course of neurodermitis and oral focus finding. Acta Stomatol Croat. 2000;1(34):89–94.
- Satoh T, Takayama K, Sawada Y, et al. Chronic nodular prurigo associated with nummular eczema: possible involvement of odontogenic infection. Acta Derm Venereol. 2003;5(83):376–377.
- Satoh T, Yokozeki H, Nishioka K. Chronic pigmented purpura associated with odontogenic infection. JAAD. 2002;6(46):942–944.
- Molin C. Amalgam—fact and fiction. Scand J Dent Res. 1992;100(1):66–73.
- Herrström P, Högstedt B. Allergic diseases, dental health, and socioeconomic situation of Swedish teenagers. Scand J Prim Health Care. 1994;12(1): 57–61.
- Schaub B, Lauener R, von Mutius E. The many faces of the hygiene hypothesis. J Allergy Clin Immunol. 2006;117(5):969–977; quiz 978.
- Okuda K, Ebihara Y. Relationships between chronic oral infectious diseases and systemic diseases. Bull Tokyo Dent Coll. 1998;39(3):165–174.
- Azizi A, Rezaee M. Comparison of periodontal status in gingival oral lichen planus patients and healthy subjects. Dermatol Res Pract. 2012;2012.
- Rai NP, Kumar P, Mustafa SM, et al. Relation between periodontal status and pre-cancerous condition (oral lichen planus): a pilot study. Adv Clin Exp Med. 2016;25(4):763–766.
- Ertugrul AS, Arslan U, Dursun R, Hakki SS. Periodontopathogen profile of healthy and oral lichen planus patients with gingivitis or periodontitis. Int J Oral Sci. 2013;5(2):92–97.
- Ramón-Fluixá C, Bagán-Sebastián J, Milián-Masanet M, Scully C. Periodontal status in patients with oral lichen planus: a study of 90 cases. Oral Dis. 1999;5(4):303–306.
- Xue JL, Fan MW, Wang SZ, et al. A clinical study of 674 patients with oral lichen planus in China. J Oral Pathol Med. 2005;34(8):467–472.
- Bajaj DR, Khoso NA, Devrajani BR, et al. Oral lichen planus: a clinical study. J Coll Physicians Surg Pak. 2010;20(3):154–157.
- Holmstrup P, Schiøtz AW, Westergaard J. Effect of dental plaque control on gingival lichen planus. Oral Surg Oral Med Oral Pathol. 1990;69(5):585–590.
- Tricamo MB, Rees TD, Hallmon WW, et al. Periodontal status in patients with gingival mucous membrane pemphigoid. J Periodontol. 2006;77(3):398–405.
- Arduino PG, Farci V, D’Aiuto F, et al. Periodontal status in oral mucous membrane pemphigoid: initial results of a case-control study. Oral Dis. 2011;17(1):90–94.
- Lo Russo L, Guiglia R, Pizzo G, et al. Effect of desquamative gingivitis on periodontal status: a pilot study. Oral Dis. 2010 Jan;16(1):102–107.
- Scully C, Carrozzo M, Gandolfo S, et al. Update on mucous membrane pemphigoid: a heterogeneous immune-mediated subepithelial blistering entity. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(1):56–68.
- Schellinck AE, Rees TD, Plemons JM, et al. A comparison of the periodontal status in patients with mucous membrane pemphigoid: a 5-year follow-up. J Periodontol. 2009;80(11):1765–1773.
- Thorat MS, Raju A, Pradeep AR. Pemphigus vulgaris: effects on periodontal health. J Oral Sci. 2010;52(3):449–454.
- Akman A, Kacaroglu H, Yilmaz E, Alpsoy E. Periodontal status in patients with pemphigus vulgaris. Oral Dis. 2008;14(7):640–643.
- Arduino PG, Broccoletti R, Sciannameo V, Scully C. A practical clinical recording system for cases with desquamative gingivitis. Br J Dermatol. 2017;177(1):299–301.
- Jascholt I, Lai O, Zillikens D, Kasperkiewicz M. Periodontitis in oral pemphigus and pemphigoid: A systematic review of published studies. J Am Acad Dermatol. 2017;76(5):975–978.e3.
- Gambino A, Carbone M, Arduino PG, et al. Conservative approach in patients with pemphigus gingival vulgaris: a pilot study of five cases. Int J Dent. 2014;2014:747506.
- Antal M, Braunitzer G, Mattheos N, et al. Smoking as a permissive factor of periodontal disease in psoriasis. PLoS ONE. 2014;9(3):e92333.
- Lazaridou E, Tsikrikoni A, Fotiadou C, et al. Association of chronic plaque psoriasis and severe periodontitis: a hospital based case-control study. J Eur Acad Dermatol Venereol. 2013;27(8):967–972.
- Nakib S, Han J, Li T, et al. Periodontal disease and risk of psoriasis among nurses in the United States. Acta Odontol Scand. 2013;71(6):1423–1429.
- Skudutyte-Rysstad R, Slevolden EM, Hansen BF, et al. Association between moderate to severe psoriasis and periodontitis in a Scandinavian population. BMC Oral Health. 2014;14:139.
- Sharma A, Raman A, Pradeep AR. Association of chronic periodontitis and psoriasis: periodontal status with severity of psoriasis. Oral Dis. 2015;21(3):314–319.
- Keller JJ, Lin HC. The effects of chronic periodontitis and its treatment on the subsequent risk of psoriasis. Br J Dermatol. 2012;167(6):1338–1344.
- Telfer NR, Chalmers RJ, Whale K, Colman G. The role of streptococcal infection in the initiation of guttate psoriasis. Arch Dermatol. 1992;128(1):39–42.
- Thorleifsdottir RH, Eysteinsdóttir JH, Olafsson JH, et al. Throat infections are associated with exacerbation in a substantial proportion of patients with chronic plaque psoriasis. Acta Derm Venereol. 2016;96(6):788–791.
- Üstün K, Sezer U, K?sac?k B, et al. Periodontal disease in patients with psoriatic arthritis. Inflammation. 2013;36(3):665-669.
- Wu W, Debbaneh M, Moslehi H, et al. Tonsillectomy as a treatment for psoriasis: a review. J Dermatolog Treat. 2014;25(6):482–486.
- Thorleifsdottir RH, Sigurdardottir SL, Sigurgeirsson B, et al. HLA-Cw6 homozygosity in plaque psoriasis is associated with streptococcal throat infections and pronounced improvement after tonsillectomy: a prospective case series. J Am Acad Dermatol. 2016;75(5):889–896.
- Johnston A, Gudjonsson JE, Sigmundsdottir H, et al. Peripheral blood T cell responses to keratin peptides that share sequences with streptococcal M proteins are largely restricted to skin-homing CD8+ T cells. Clin Exp Immunol. 2004;138(1):83–93.
- Valdimarsson H, Sigmundsdóttir H, Jónsdóttir I. Is psoriasis induced by streptococcal superantigens and maintained by M-protein-specific T cells that cross-react with keratin? Clin Exp Immunol.
1997;107 Suppl 1:21-24.